The eye as an organ is composed of specific types of tissues and structures that are not found anywhere else in our body (e.g. cornea and vitreous), but also of some others that are not specific for any organ, but are found in most or all organs ( blood vessels, nerves, connective tissue). Therefore, it is easy to conclude that certain diseases of certain tissues or structures affect these tissues in all parts of the body, wherever they are, including in the eye.
Diabetes
Diabetics are more likely to suffer from barley and inflammation of the eyelids. The reason for this is a disturbed metabolism and the development of bacteria that cause inflammation. Burning and stinging of the eye or true conjunctivitis also sometimes occurs in diabetics, and their partial cause is again an increased concentration of sugar in the tears. In severe forms of diabetes, in which there is nerve involvement (polyneuropathy), the sensitivity of the cornea decreases, which eliminates one of its main protective mechanisms. Namely, the stimulation of the cornea causes reflex blinking and wetting of the eye with tears, which protects the cornea from adverse environmental factors. When this reflex disappears, its damage, drying and inflammation occur much more often. In long-term diabetes, newly formed blood vessels can be found on the iris, which is particularly evident in proliferative diabetic retinopathy. It should be emphasized that diabetes affects the lens of the eye even before the formation of cataracts, in such a way that due to changes in sugar concentration, there are changes in the amount of water in the lens. This changes its transparency and degree of light refraction, so the vision of these patients is sometimes better and sometimes worse. It is not possible to predict if and when diabetics will develop cataracts. This depends on a large number of factors, one of the most significant of which is the success of maintaining blood sugar within normal limits. Diabetics with extremely high blood sugar can develop cataracts in a very short period of time, but this is still rare. It is much more common that diabetes only accelerates the development of cataracts in people who would have developed them anyway. We are witnessing more frequent bleeding into the vitreous body. This is a disorder of the wall of all the blood vessels of the eye’s background, especially the newly formed ones (in proliferative diabetic retinopathy). When they break, the blood is localized only in some layers of the retina or is mixed with the vitreous. In this case, there is a sudden loss of vision, and the severity of this loss depends on the amount of blood shed.
Changes in the fundus of the eye are described under “Diseases of the retina”.
Dysthyroid orbitopathy
Origin of the disease:
Dysthyroid orbitopathy is a disease of the eye and its surrounding and associated structures that is associated with thyroid disease. Namely, in diseases of the thyroid, in which there is an increase in the secretion of its hormones, changes in the tissues of the orbit often occur in parallel. This is proven by statistics that show that almost 80% of orbitopathies occur in hyperthyroidism (a state of increased secretion of thyroid hormones), but in the remaining 20% they occur in states with normal or even reduced thyroid function. The causes of this connection are only partially clarified, and they mainly lie in the fact that the antibodies that cause thyroid disease also affect some tissues around the eye that have a thyroid-like structure. In a simplified way, it can be said that it is a pathology of the immune system.
Symptoms:
The symptoms of hyperthyroidism are mostly known (weight loss, fatigue, rapid heartbeat, nervousness, hair loss, rapid and/or hoarse speech), so here we will concentrate only on the eye symptoms.
Protrusion of the eyeball, a condition in which the eye is pushed forward, is caused by an increase in the content of the orbit due to the accumulation of water in fatty tissue and muscles. It is associated with retraction of the eyelids, i.e. the pulling of the upper eyelids upwards, which gives the impression that the eyes are even more open. Such a patient sometimes cannot even close the eyelids completely and even sleeps with “open” eyes. This, as well as the fact that blinking is less common in this disease, directly affects the reduction of the protection of the cornea and its drying, which results in small damages on the surface that cause itching and burning. Swelling of fatty tissue and muscles has an effect on the weakening of the function of the optic nerve, partly mechanically and partly due to altered circulation. Because of this, there is a weakening of visual acuity and changes in the field of vision. At the same time, the muscles become thicker and stiffer, so in more severe cases, double vision occurs, and due to pressure on the eyeball, increased eye pressure occurs. The latter is especially pronounced in certain positions of the eye. .
Establishing a diagnosis:
Findings of thyroid hormones, which include TSH (thyroid-stimulating hormone), T3 and T4, are of key importance in determining the cause of eye changes. Ultrasound of the thyroid gland is also routinely performed, and sometimes other tests are also performed.
From eye examinations, it is necessary to determine visual acuity, an examination of the entire eye with special emphasis on the cornea and optic nerve, field of vision and measurement of eye pressure. Specific tests performed in this case are ultrasound of the eye muscles and other orbital tissue, which shows possible thickening of the muscles. The second test is measuring the protrusion of the eyeball using the Hertel method. With this method, the protrusion of the eyeball can be determined simply and accurately using the mirror system. Normal values are around 15-17 mm, and higher values or a difference in the findings between the two eyes speak in favor of orbitopathy. Both of these last-mentioned findings are not only important in diagnosing the disease, but also in monitoring the course and success of the treatment, because successful treatment reduces edema of the muscles and fat tissue of the orbit, and the eyeball returns to its place.
Treatment:
The thyroid should be treated primarily because its disorder is the cause of eye problems. The choice of therapy is up to the specialist endocrinologist, but the ophthalmological findings are certainly taken into account. It primarily consists of thyrostatics in cases of hyperthyroidism, i.e., hormone replacement in those rare cases when insufficient thyroid hormone secretion is the cause of orbitopathy. With hyperthyroidism, treatment with radioiodine, surgical removal of part of the thyroid gland, and some other types of therapy are also considered.
Local attention should primarily be focused on the existence of dry eyes and related corneal defects. The treatment is carried out with drops of artificial tears that create a thin film over the cornea that protects the eye and reduces friction between the cornea and the eyelids when blinking, and if necessary, other means with a similar effect. When glaucoma occurs, the treatment described under the category “Glaucoma” is carried out. It should be emphasized that severe and serious increases in intraocular pressure are less common.
More severe forms of orbitopathy are treated with corticosteroid drugs that have a strong anti-inflammatory effect, and which are given as injections behind the eye (behind the eyeball, retrobulbar). Injections are administered consecutively for 10 days. Another way of administering corticosteroid drugs is through infusion, which achieves significantly higher concentrations of the drug both in the entire circulation and in the eye area. This method is reserved only for the most severe forms of the disease.
After the hormonal status and eye findings have calmed down, if the eyes are still to an unacceptably large extent protruding forward, part of the fat tissue of the orbit can be surgically removed. With this procedure, the eyeball is pulled back. The technique is applied through the upper and lower eyelids, and more recently, the endoscopic method through the nose. To eliminate certain changes associated with muscle tension and eyelid retraction, Botulinum toxin preparation is used in the form of injections, which has a temporary effect, or certain surgical procedures with a permanent effect.
It is also possible to reduce the volume of the orbital tissue with radioactive radiation.
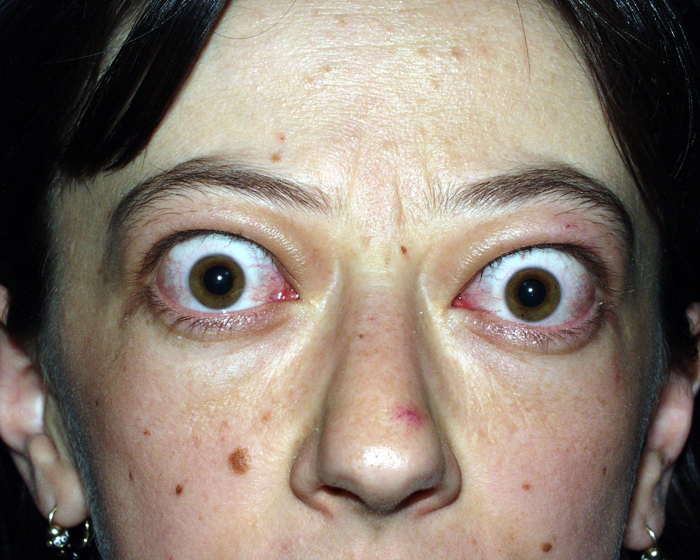
A patient with dysthyroid orbitopathy
Literature:
M.Sc. sc. Pavan Dr. Joško, “Eye Diseases”, Zagreb 2003.








